IUD CONTRACEPTION

INTRA-UTERINE DEVICE (IUD) -THE SAFEST FORM OF CONTRACEPTION!
Are you looking for a form of birth control that is safe, effective, has an option of no hormones, and is hassle free? Look no further than the IUD!
WHAT IS AN IUD?
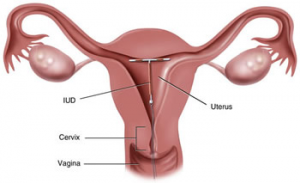
- An IUD is a small T-shaped plastic device that fits snugly inside your uterus.
- An IUD can simply be put into the uterus through the cervix, during a regular vaginal examination.
- In Canada, there are 2 types of IUD’s, one coated with copper and the other with progesterone hormone. In other countries there are many types and shapes.
- None of the IUD’s have estrogen hormone.
There are many stories and myths about IUD’s enough to scare anyone… This is because in the early 1970’s there was a poorly designed IUD (the dreaded “Dalcon Shield” which caused infections, thus giving all IUD’s a bad reputation. In 1974 the Dalcon Shield was taken off the market. An advertising campaign to get women to have the Dalcon Shield removed, resulted in a negative image and stigma to all IUD’s in North America. Since that time, IUD’s have been redesigned and for women around the world, IUD’s are now the most commonly used form of reversible contraception. They are by far the safest and most reliable form of contraception when used in the right setting.
DID YOU KNOW?
That IUD’s used today have fewer accidental pregnancies than the Pill or even a Tubal Ligation? (If you use the Pill or have a Tubal Ligation (your tubes tied) you can still sometimes get pregnant). That you can safely use an IUD as your first type of contraception. That you can use an IUD if you are Breast Feeding. Using an IUD is hassle free, without having to remember to take a pill every day. That an IUD can be put in at the same time that you have treatment for a miscarriage or an abortion. Mirena IUD’s make your periods much lighter with less cramping. Copper IUD’s do not change your hormone levels! IUDs can improve your sex life. If you are in a safe, committed relationship you may feel more spontaneous without the worry of becoming pregnant. IUD’s are private. No one knows that you use contraception. There are no packages left lying around!
HOW DOES IT WORK?
IUD’s mainly prevent the sperm from reaching your egg in the fallopian tube. This is achieved by creating a mild inflammatory response in the uterus which prevents the sperm from reaching the egg. It is unlikely that an egg is ever fertilized. The Mirena IUD also thins the lining of the uterus and causes the fluid in the cervix to become thicker which helps prevent sperm from entering the uterus.
CAN I USE AN IUD IF I HAVE NEVER BEEN PREGNANT?
YES! (We need to make sure that your uterus is big enough to fit an IUD. We will measure the uterus length using an Ultrasound beforehand.
CAN I HAVE AN IUD INSERTED AFTER I HAVE HAD A BABY?
Yes, but this is usually done after about 6 weeks, to give your uterus and cervix time to shrink back to normal size. If we put it in too soon, the IUD can fall out
I AM A TEENAGER… CAN I USE AN IUD?
YES, as long as you do not have multiple partners or have other increased risks of sexually transmitted infections, just like any other woman interested in using an IUD.
WILL MY PARTNER FEEL THE STRINGS DURING SEX?
- Usually not, but if he does, we can shorten the strings for you.
- Please make sure that your partner does not pull on the strings during foreplay with his / her fingers!
HOW ABOUT USING AN IUD FOR EMERGENCY CONTRACEPTION, LIKE PLAN B?
- Copper IUD’s can be used as a form of emergency contraception to prevent a pregnancy if inserted within 3 to 5 days after having unprotected sex.
- This can prevent a pregnancy now and for the future!
WHICH OF THE 2 IUD’s IN CANADA SHOULD I USE?
- The Copper IUD (Flexi T and Novo T) has a copper coating. It is hormone free.
- It lasts for 4-3-5 years.
- The Copper IUD can sometimes cause your periods to be heavier with more cramps.
- It costs about $170.
- The Mirenaand Jaydess IUD have a progesterone hormone coating.
- If you already have heavier periods, the progesterone coating thins the lining of the uterus and results in lighter periods (up to 90% lighter).
- There is a small chance that your period may go away after 6 months.
- There is usually no increased cramping and often period cramps improve.
- The MirenaIUD lasts for 5 years and the Jaydess is for 3 years.
- The Jaydess is slightly smaller than the Mirena IUD and has less progesterone hormone.
- Initially, you may experience random spotting for up to 4 months, although this does not always happen.
- It costs around $420 for the Mirena IUD and $350 for the Jaydess IUD. Copper IUD’s range in price up to $200. (still cheaper than the Pill which costs over $1000 per 5 years).
- A benefit of the Mirena and Jaydess IUD is lighter periods; it is a common belief that light/no periods are unhealthy. In fact, if you bleed too much during periods, you loose iron with your blood and develop iron deficiency which can make you tired or drained. This is a common problem in women who have regular or heavier periods and who delay or space pregnancies. A women’s body and hormones are designed for pregnancy which naturally is followed by breast feeding. Both of these functions naturally stop your periods until you stop breast feeding. Therefore, having fewer periods is not unhealthy. In fact, you were designed to have fewer periods.
| Type | Copper IUD | Mirena/Jaydess IUD |
| How does it work? | Has a copper coating which prevents a pregnancy by reducing the activity of sperm and prevents fertilization. This is due to an inflammatory response created by the IUD. | A;Mirena/Jaydess IUD;is an estrogen free IUD that is coated with Progesterone. It works by:
|
| ; Can I still get pregnant? | Less than 1% | Less than 1 % |
| ; How long can I keep it in? | Up to 5 years | Up to 5 years for the Mirena and 3 years for the Jaydess IUD |
| ; When can I have it removed? | Anytime you wish | Anytime you wish |
| ; Can I get pregnant soon after it is removed? | YES | There may be a lag time of a few months |
| ; Will my periods be heavier or lighter? | Can be heavier | Lighter |
| ; Any spotting between periods? | Generally not | Can happen for the first 4-6 months |
| ; Can my period disappear? | No | After a 4 -6 months, you may have less bleeding or sometimes no periods (less than 25% of women). This is not a problem! ; |
| ; Can I get worse period pain or cramping? | Yes | No, often less cramping occurs. |
| ; Will the copper affect me | NO, very small amounts are released | N/A |
| ; Will the progesterone affect me? | N/A | Because the Mirena or Jaydess IUD slowly releases very small amounts of progesterone, some women can experience side-effects. These are rare but can include: headache, breast tenderness, acne. This is much less of a problem than if you used the pill and usually disappears after 1 to 2 months. ; |
| ; Can I use it if I am breast feeding? | Yes, once your milk is established | Yes, once your milk is established |
| ; Can I use it if I have had Breast Cancer? | Yes | Likely NO |
| ; If I get pregnant, can I have a tubal pregnancy? | Yes, there is a small chance of a pregnancy being in the tube. (see below) | |
| ; Should I still use condoms? | YES, especially if you are in a new relationship or have more than one partner. This protects you from infections! ; | |
| ; Is there an increased risk of uterus cancer? | No, both IUD’s may be protective against uterus cancer | |
WHEN SHOULD I NOT USE AN IUD?
- If you have unexplained vaginal bleeding or an abnormally shaped uterus.
- If you currently have PID or an STD or have multiple episodes of these infections.
- If you have sexual behaviour putting you at risk of STD’s or PID. (e.g. multiple partners without reliably using condoms).
- Following a recent infection (within 3 months) of the uterus lining (endometritis) due to a delivery or an abortion.
- If an IUD has fallen out. (because there is a 30% chance if it happening again) We will discuss this with you to evaluate if an IUD can be used again.
- Allergy to copper or if you have a rare disease affecting copper metabolism (Wilson’s Disease).
- If you have untreated HIV, uncontrolled Diabetes or use medication that affects your immune system. (e.g. steroids).
- If you have an artificial heart valve or joint.
- If you have a bleeding abnormality (bleed too much)
- If you use medicine to thin your blood.
WHAT ARE THE RISKS OR COMPLICATIONS WHEN USING AN IUD?
Like anything we do, there are always small risks, some more serious than others. Remember that over 100 million women use IUD’s, the vast majority without any complications. However, we want you to be fully informed of all the risks that can happen, even if they are very, very rare.
- You can rarely get pregnant with an IUD. This happens less than 1% of the time. [You will not get pregnant 99% of the time if you use an IUD!] (this compares with 3 – 5% if you use the Pill and similar or even a little safer than having your tubes tied.
If you get pregnant when using an IUD, there is an increased chance of having a tubal pregnancy (ectopic). This risk is still much lower (half the chance) than having an ectopic pregnancy if you used no contraception. Ectopic pregnancies are in the tube rather than in the uterus. Ectopic pregnancies are dangerous and always have to be treated to prevent bleeding.
WARNING SIGNS
- Irregular vaginal bleeding
- Pain in the pelvis, abdomen or tip of the shoulder
- Sudden dizziness, weakness or fainting
- Copper IUD’s can sometimes cause heavier and more painful periods.
- You can have spotting when using the Mirena IUD for the first few months.
- If you have multiple partners, or if your partner has other sexual partners without reliable condom use, you are at risk of developing STD’s or Pelvic Infection (PID = Pelvic Inflammatory Disease). We do not recommend using an IUD in these circumstances. If you are not at risk for STD’s (sexually transmitted infection like Chlamydia and Gonorrhea), then an IUD should not increase your risk of getting a pelvic infection.
- If you are immuno-compromised, such as untreated HIV, poorly controlled Diabetes or using medications that interfere with your ability to fight infections, we do not recommend the IUD because of the risk of infection.
- There is a very small risk that the IUD can be expelled or fall out during the first year. This is more common during the first 3 months after insertion, if you have not already been pregnant, if you have fibroids or if you have an abnormal uterus shape. That is why we recommend that you feel for the IUD string in your vagina once a month.
- There is a small increased risk of infection during the first 3 weeks after insertion. Some authorities recommend using condoms for the first 3 -4 weeks to limit this risk.
- During the insertion of the IUD, it can accidentally pass through the wall of the uterus (perforate) and land inside the pelvis and sometimes can damage surrounding organs. This will need to be removed by way of an operation. Perforation is very rare. If you have severe pain during insertion, please let the doctor know! There is also a very small chance that the IUD can migrate through the wall of the uterus over time.
WHEN IS IT INSERTED?
- It can be inserted anytime if you are using the Pill or Nuvaring.
- If you are not using any other hormonal contraception, we usually insert it during a period to ensure that you are not already pregnant and because it is easier at that time, however, on rare occasions, we can insert it anytime if you are not pregnant.
- It can safely be inserted immediately after treatment for an early miscarriage or abortion provided there is no infection.
HOW IS IT PUT IN?
- An IUD is inserted during a vaginal examination similar to that when you have a pap test.
- We take cultures beforehand to make sure there is no infection. If we do not have the results back in time, we will likely offer you a course of antibiotics once the IUD is inserted.
- At Meridia Gynecology, we always give you an anti-inflammatory tablet beforehand, and use a small amount of local anaesthetic at your cervix to make the process more comfortable.
- The vagina and cervix are cleaned with antiseptic solution to minimize any infection that can occur during insertion.
- The IUD is then gently passed through the cervix into the uterus.
- There is a small string attached to the bottom of the IUD; this allows us (you and your doctor) to check that it remains in place. The string (nylon thread) is visible at your cervix (the bottom part of your womb). Your cervix can be felt if you put your finger deep into your vagina (best felt when squatting), it feels firm and moves around like the tip of your nose.
- Once the IUD is in place, we shorten the strings and usually do an ultrasound to ensure that it is in the correct position.
- There should only be minimal discomfort when the IUD is inserted correctly.
WHAT SHOULD I BE CHECKING FOR AFTER THE IUD HAS BEEN INSERTED?
You need to monitor for signs of infections (especially during the first 3 weeks), the IUD falling out or incorrectly positioned and the rare chance of becoming pregnant, especially an ectopic pregnancy. Symptoms include:
- Pelvic pain or tenderness in the lower abdomen.
- Fever, vomiting or diarrhea.
- Heavy bleeding or prolonged bleeding.
- New irregular bleeding (need to make sure there is nothing else causing this).
- Symptoms of pregnancy (see below about pregnancy).
- If any of these occur, please come in immediately, or go to your Family Doctor or to the ER after hours.
- Please check for the strings after your periods to make sure that the IUD is still in place. (Don’t panic if you can’t feel them, sometimes the strings hide inside the cervix. Just come in and we will look for them or do an ultrasound if necessary).
YOUR NEXT APPOINTMENT AFTER THE IUD IS INSERTED?
- We will like to see you in 1 month to shorten the strings if need be and make sure that the IUD is in place. We can discuss any side effects you may be having.
IF I THINK THAT I AM PREGNANT WITH THE IUD?
- If you think that you may be pregnant, or have symptoms of being pregnant (miss a period, nausea, breast tenderness /enlargement; morning sickness etc) have a pregnancy test immediately, and repeat it weekly until your period comes or if the test is negative for 2 weeks in a row.
- If your periods disappear when using the Mirena or Jaydess IUD, you will have to rely on other symptoms of pregnancy in the rare event that you become pregnant. (Breast tenderness, breast enlargement, nausea, morning sickness, new spotting etc).
- If you are pregnant, you will need a blood test as well as ultrasounds to make sure you do not have an ectopic pregnancy. Please have this done immediately if you are pregnant. Ectopic pregnancies can be dangerous to your health, and always have to be treated.
- If you become pregnant with an IUD in place, and the pregnancy is in the uterus, the IUD should be removed immediately to prevent the risk of severe infection, miscarriage and premature birth. There is a chance that a miscarriage may happen after the IUD has been removed.
- If this is not a planned pregnancy, you may choose to have an abortion at our centre. See our “Pregnancy choice” information in the Gyne Topics section.
- If it is too late or the IUD cannot be removed, then you will need careful monitoring during the pregnancy.
WHY DO YOU GET PREGNANT WHEN USING AN IUD?
- The IUD sometimes falls out of the uterus (always check for the strings).
- The IUD can migrate (very rarely) through the wall of the uterus and will not be effective.
- There is a very small chance of getting pregnant even if the IUD is in the correct position. (less common than the Pill or even a tubal ligation).
TAKING OUT OR REPLACING THE IUD?
- We can take out the IUD any time you want it removed.
- IUD’s need to be replaced within 3-5 years to ensure that they are still effective and to avoid infections.
